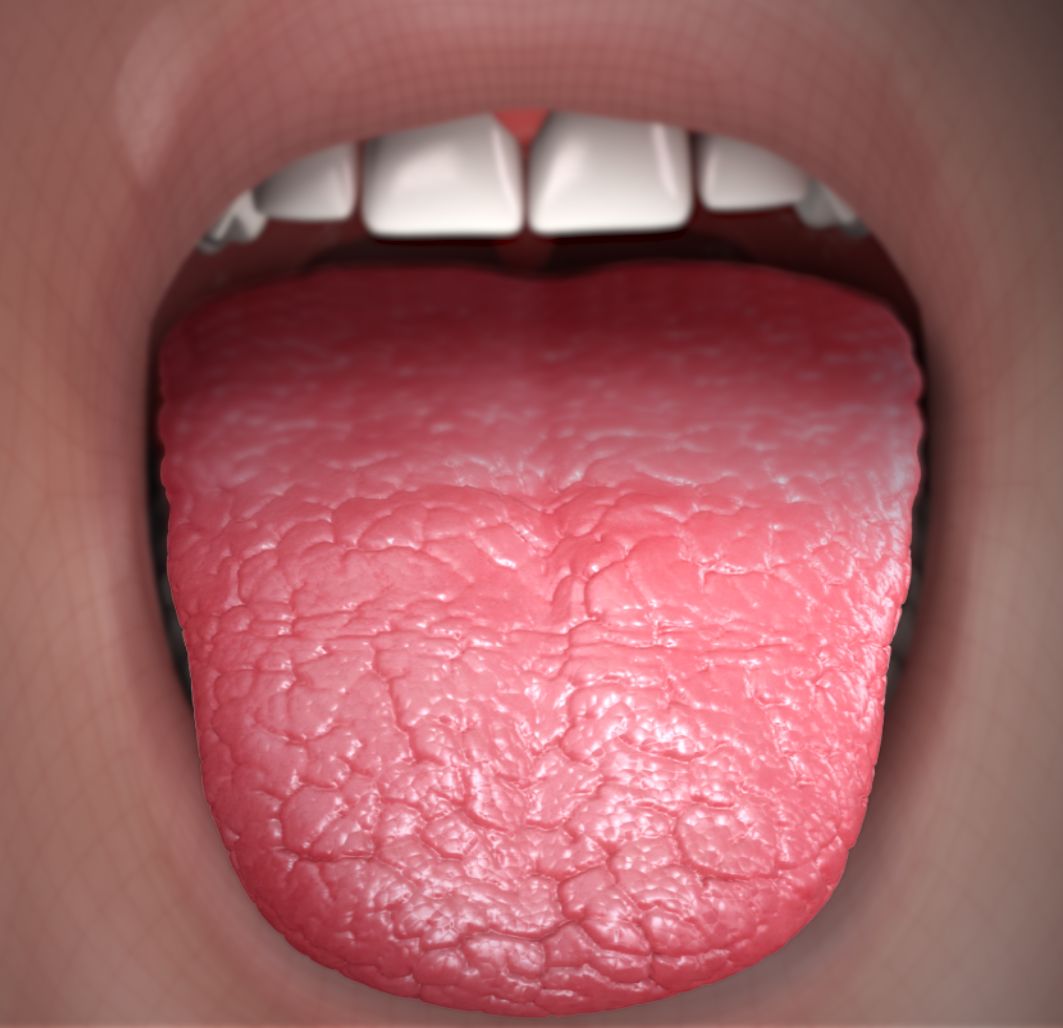
Xerostomia
Medical condition
Xerostomia, also known as dry mouth, is a subjective complaint of dryness in the mouth, which may be associated with a change in the composition of saliva, reduced salivary flow, or have no identifiable cause.
This symptom is very common and is often seen as a side effect of many types of medication. It is more common in older people (mostly because individuals in this group are more likely to take several medications) and in people who breathe through their mouths. Dehydration, radiotherapy involving the salivary glands, chemotherapy and several diseases can cause reduced salivation (hyposalivation), or a change in saliva consistency and hence a complaint of xerostomia. Sometimes there is no identifiable cause, and there may sometimes be a psychogenic reason for the complaint.
Definition
Xerostomia is the subjective sensation of dry mouth, which is often (but not always) associated with hypofunction of the salivary glands. The term is derived from the Greek words ξηρός (xeros) meaning "dry" and στόμα (stoma) meaning "mouth". A drug or substance that increases the rate of salivary flow is termed a sialogogue.
Hyposalivation is a clinical diagnosis that is made based on the history and examination, but reduced salivary flow rates have been given objective definitions. Salivary gland hypofunction has been defined as any objectively demonstrable reduction in whole and/or individual gland flow rates. An unstimulated whole saliva flow rate in a normal person is 0.3–0.4 ml per minute, and below 0.1 ml per minute is significantly abnormal. A stimulated saliva flow rate less than 0.5 ml per gland in 5 minutes or less than 1 ml per gland in 10 minutes is decreased. The term subjective xerostomia is sometimes used to describe the symptom in the absence of any clinical evidence of dryness. Xerostomia may also result from a change in composition of saliva (from serous to mucous). Salivary gland dysfunction is an umbrella term for the presence of xerostomia, salivary gland hyposalivation, and hypersalivation.
Signs and symptoms
Hyposalivation may give the following signs and symptoms:
- Dental caries (xerostomia related caries) – Without the buffering effects of saliva, tooth decay becomes a common feature and may progress much more aggressively than it would otherwise ("rampant caries"). It may affect tooth surfaces that are normally spared, e.g., cervical caries and root surface caries. This is often seen in patients who have had radiotherapy involving the major salivary glands, termed radiation-induced caries. Therefore, it is important that any products used in managing dry mouth symptoms are sugar-free, as the presence of sugars in the mouth support the growth of oral bacteria, resulting in acid production and development of dental caries. In addition, reduced salivary flow and altered composition can result in a lowered buffering capacity and pH, which contributes to dental caries and tooth surface demineralization. Research shows that enamel demineralization typically begins when oral pH drops below about 5.5, while root dentin, being more vulnerable, can start to erode at a higher pH of around 6.7. Many saliva substitutes and oral moisturizers are formulated with a pH below 6.7, which can pose a risk to dentin over time.
- Acid erosion. Saliva acts as a buffer and helps to prevent demineralization of teeth.
- Oral candidiasis – A loss of the antimicrobial actions of saliva may also lead to opportunistic infection with Candida species.
- Ascending (suppurative) sialadenitis – an infection of the major salivary glands (usually the parotid gland) that may be recurrent. It is associated with hyposalivation, as bacteria are able to enter the ductal system against the diminished flow of saliva. There may be swollen salivary glands even without acute infection, possibly caused by autoimmune involvement.
- Dysgeusia – altered taste sensation (e.g., a metallic taste) and dysosmia, altered sense of smell.
- Intraoral halitosis – possibly due to increased activity of halitogenic biofilm on the posterior dorsal tongue (although dysgeusia may cause a complaint of nongenuine halitosis in the absence of hyposalivation).
- Burning mouth syndrome – a burning or tingling sensation in the mouth.
- Saliva that appears thick or ropey.
- Mucosa that appears dry.
- A lack of saliva pooling in the floor of the mouth during examination.
- Dysphagia – difficulty swallowing and chewing, especially when eating dry foods. Food may stick to the tissues during eating.
- The tongue may stick to the palate, causing a clicking noise during speech, or the lips may stick together.
- Gloves or a dental mirror may stick to the tissues.
- Fissured tongue with atrophy of the filiform papillae and a lobulated, erythematous appearance of the tongue.
- Saliva cannot be "milked" (expressed) from the parotid duct.
- Difficulty wearing dentures, e.g., when swallowing or speaking. There may be generalized mucosal soreness and ulceration of the areas covered by the denture.
- Mouth soreness and oral mucositis.
- Lipstick or food may stick to the teeth.
- A need to sip drinks frequently while talking or eating.
- Dry, sore, and cracked lips and angles of mouth.
- Thirst.
However, sometimes the clinical findings do not correlate with the symptoms experienced. For example, a person with signs of hyposalivation may not complain of xerostomia. Conversely a person who reports experiencing xerostomia may not show signs of reduced salivary secretions (subjective xerostomia). In the latter scenario, there are often other oral symptoms suggestive of oral dysesthesia ("burning mouth syndrome"). Some symptoms outside the mouth may occur together with xerostomia.
These include:
- Xerophthalmia (dry eyes).
- Inability to cry.
- Blurred vision.
- Photophobia (light intolerance).
- Dryness of other mucosae, e.g., nasal, laryngeal, and/or genital.
- Burning sensation.
- Itching or grittiness.
- Dysphonia (voice changes).
There may also be other systemic signs and symptoms if there is an underlying cause such as Sjögren's disease, for example, joint pain due to associated rheumatoid arthritis.
Cause
The differential of hyposalivation significantly overlaps with that of xerostomia. A reduction in saliva production to about 50% of the normal unstimulated level will usually result in the sensation of dry mouth. Altered saliva composition may also be responsible for xerostomia.
Physiological
Salivary flow rate is decreased during sleep, which may lead to a transient sensation of dry mouth upon waking. This disappears with eating or drinking or with oral hygiene. When associated with halitosis, this is sometimes termed "morning breath". Dry mouth is also a common sensation during periods of anxiety, probably owing to enhanced sympathetic drive. During periods of stress, our body responds in a 'fight or flight' state that will interfere with the saliva flow in the mouth. Dehydration is known to cause hyposalivation, the result of the body trying to conserve fluid. Physiologic age-related changes in salivary gland tissues may lead to a modest reduction in salivary output and partially explain the increased prevalence of xerostomia in older people. However, polypharmacy is thought to be the major cause in this group, with no significant decreases in salivary flow rate being likely to occur through aging alone.
Drug induced xerostomia
Aside from physiological causes of xerostomia, iatrogenic effects of medications are the most common cause. A medication which is known to cause xerostomia may be termed xerogenic. Over 400 medications are associated with xerostomia. Although drug induced xerostomia is commonly reversible, the conditions for which these medications are prescribed are frequently chronic. The likelihood of xerostomia increases in relation to the total number of medications taken, whether the individual medications are xerogenic or not. The sensation of dryness usually starts shortly after starting the offending medication or after increasing the dose. Anticholinergic, sympathomimetic, or diuretic drugs are usually responsible.
Sjögren's syndrome
Xerostomia may be caused by autoimmune conditions which damage saliva-producing cells. Sjögren's syndrome is one such disease, and it is associated with symptoms including fatigue, myalgia and arthralgia. The disease is characterised by inflammatory changes in the moisture-producing glands throughout the body, leading to reduced secretions from glands that produce saliva, tears and other secretions throughout the body. Primary Sjögren's syndrome is the combination of dry eyes and xerostomia. Secondary Sjögren's syndrome is identical to primary form but with the addition of a combination of other connective tissue disorders such as systemic lupus erythematosus or rheumatoid arthritis.
Celiac disease
Xerostomia may be the only symptom of celiac disease, especially in adults, who often have no obvious digestive symptoms.
Content sourced from Wikipedia under CC BY-SA 4.0